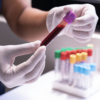
With its newest location in Vancouver, Field Trip Health Ltd (CSE: FTRP) (OTCQX: FTRPF) is growing its footprint of clinics, which feature psychotherapy aided by mind-expanding substances.
After opening its first location in Toronto in June 2020, the company has added seven locations in major U.S. cities, three in Canada and one in the Netherlands.
In Canada, its services focus on a program of psychotherapy aided by sessions of taking ketamine, an anesthetic and painkiller primarily used in veterinary work that has become a popular club drug for its dissociative, dance-friendly effects.
But according to research, and results from companies like Field Trip, the substance can be a powerful therapeutic tool that can lead to lasting benefits not seen with conventional methods.
Read more: Field Trip white paper makes strong health and business case for ketamine therapy
As its Vancouver location opens this week, founder and executive chairman Ronan Levy talks to Mugglehead about what the new clinic will offer, why physicians are more open-minded about ketamine than cannabis as well as the balance between profit and accessibility in new-age health care services.
The following interview has been edited for length and clarity.
You have a presence in Canada, the U.S. and Amsterdam. What kind of differences do you notice market-to-market, and then coming to Vancouver, what do you expect here? Are you going to be tailoring your services, or are they going to be pretty much the same across locations?
Vancouver is actually going to be a unique location for us. In all of the other Canadian and U.S. locations, we’re doing ketamine-assisted therapy. In the Netherlands, we’re doing psilocybin-assisted therapy. But what’s unique about Vancouver is that we’re going to start piloting other modalities as well.
We’ll be providing ketamine-assisted therapy for sure, but we’ll also start offering RMT services, hosting yoga classes — other kinds of health-related therapeutic techniques will be offered. As it starts to operate it won’t launch with that but those are plans.

Before launching Field Trip in 2018, Ronan Levy was a co-founder and director at CanvasRx (the company behind cannabisclinics.ca) and a senior VP at Aurora Cannabis. Submitted photo
So your ketamine-assisted therapy program, CORE, will be the main focus at the clinic?
Yeah. Initially, we started off with pretty structured programs where a person would go through four or six sessions in a fairly specific timeframe, now it’s become a little more flexible because scheduling challenges made it hard for people to adhere to those programs.
In our CORE program, most people who come in are experiencing treatment-resistant depression. You see the best results when they have four-to-six ketamine sessions. Typically what we do is an initial screening with a psychiatrist to make sure ketamine-assisted therapy is appropriate. There’s a preparatory session with your therapists and therapeutic team.
You have your first ketamine-assisted therapy session, and then following that there are about 30 minutes of integration therapy. And then typically you’d have two ketamine sessions, followed by one integration session. And that’s spaced out over maybe two ketamine sessions in the course of a week.
And then earlier the following week you do an integration session. During the integration session, there’s no ketamine. It’s just taking the window of neuroplasticity that follows the ketamine experience, and really trying to put that into behaviour change, outlook change, mindset change — all the things that support the mood improvements that come from the ketamine itself.
What are your main target audiences? And how are you reaching more people in those different audiences?
Our target person is someone who has experienced some level of treatment-resistant mental health challenge, whether that’s depression, anxiety, trauma or PTSD. For anyone who’s tried conventional approaches and hasn’t had success, I think ketamine-assisted therapy should be an option because we’re seeing just remarkable results. People with eating disorders can benefit from these kinds of therapies as well.
Do you have like a typical client lifecycle? I’m guessing some clients who get a lot out of one round of therapy. But I imagine you also have some who will have that and then probably return over a period of time.
It’s really hard to say to be honest. Our Toronto clinic has only been operating since last June so we didn’t have that many patients initially. But what we’re seeing is people typically complete the CORE program. And then about a handful of maybe like 20–30 per cent have since come back to do a single session — one ketamine session and one integration. Once and then maybe a few months later another one, so they’re treating it more like a maintenance approach as opposed to a transformative therapeutic approach, which is what the initial experience tends to be like.

Field Trip will be piloting a number of health and wellness services, like yoga, at its Vancouver location
From a business standpoint, when you’re talking about this mix of services in Vancouver, is that part of like galvanizing your existing client base? As in, you have people that go through the ketamine program but then you have all these other services, and so they keep coming in? Or is it more that there’s just a bigger range of services, so you’re bringing more people in, and then educating them about all the other stuff you offer? Or both?
Yeah, I think it’s bi-directional. By being able to offer additional services, I think we can support people better — hopefully helping them achieve a level of mental and emotional health in a very constructive way. And if they want to continue on with other activities or services, we hopefully extend those benefits. Conversely, though, psychedelic-assisted therapy is not new, but it’s a relatively new conversation for a lot of people. So if there are ways we can find to engage people in a meaningful way that gives us an opportunity to at least educate them on what’s happening and the availability of the services, we certainly would.
I know that you have a background in medical cannabis, and there’s a huge uphill battle there on the physician side that a vast majority either don’t know about it or still have a large amount of stigma toward it. In Canada, Field Trip relies on physicians directing patients to your services to a large degree. So is there a lot of work on your end, like reaching out to different physicians saying, ‘Here’s what we offer, here’s the evidence behind it,’ etc.
Yeah, absolutely. A couple of comments: when it came to cannabis, yes, there’s certainly a lot of resistance from physicians. And with Canadian Cannabis Clinics what we focused on doing was doing really good medicine. What that meant was treating patients where it’s appropriate, not prescribing cannabis where it wasn’t appropriate, following up with the referring physicians, making sure that referring physicians were part of the ongoing dialogue. We treated cannabis like every other specialty of medicine, which I think a lot of cannabis clinics did not. And that’s why we’re so effective at getting the medical community on board.
Read more: Canada’s flawed medical cannabis regime sees drop in client registrations
With ketamine, it’s the same playbook for us, which is we’re focused on doing good medicine, treating people in need, showing great results, keeping the referring physician in the loop and part of the process. But I think the resistance to what we’re doing ketamine has actually been lower than cannabis because even though it’s an off-label use, ketamine is a prescribed drug, comes with a [drug identification number], titrating it is well known and not a surprise to a lot of people. Many doctors work with ketamine.
So I think there’s just a level of understanding that goes with it, and a level of familiarity makes it an easier conversation, as well as the need. Speak to most family doctors, they’ll tell you that antidepressants are working for their patients, and they need alternatives.
In Canada, your offerings are mostly restricted to ketamine. But in Amsterdam, for example, you have a program with therapeutic psilocybin. And I know that there’s advocacy work going on in Canada from organizations like TheraPsil to have that sort of more available here as well. So is Field Trip involved in any advocacy work related to that? And would you like to offer the services here as well?
Yes we are and yes we would. We’re a part of the Canadian Psychedelic Association — one of the founding members. We’ve done a lot of education work with members of parliament. Part of the conversation that’s actually been precipitated by the review of the medically assisted dying legislation.
Everyone we’ve spoken to on a political level really resonates with the argument that if it’s a right in Canada that you can take a drug that will end your life, how can it make sense not to enable people to have access to a drug that may make the dying process much easier, more pleasant or significantly less anxiety-inducing?
It’s also a drug that helps military veterans deal with the PTSD of being at war. And so there seems to be a lot of open mindedness to it. Given that, we wouldn’t be surprised if we see some sort of regulatory change, at least for people in palliative care, next year.
Read more: Advocacy group drafts medical psilocybin framework for regulated access
Read more: Common antidepressant escitalopram and psilocybin can be taken together safely: study
So we’ve spoken with (Field Trip medical director) Dr. Michael Verbora previously on the double-edged nature of profit motives in a healthcare setting. Obviously, with money comes research and more availability, but at the same time, there’s also opportunity for helpful therapy that can be offered to like a wide variety of people, not just upper-middle class and above. What are your thoughts on that? How do you balance business objectives with making things accessible and doing a public good?
There’s no single solution to balancing access. Money is fundamentally an energy that enables growth, and we need more providers, we need more spaces, we need more research. Having a for-profit entity helps generate that funding.
I think it’s really important to keep in mind that the biggest cost associated with psychedelic-assisted therapies is not the drugs, it’s the fact that you have doctors and therapists, many or all of whom have advanced degrees and designations, spending a lot of time with people.
Anytime you have anything so labour intensive, it’s going to inherently become expensive, because people want to be paid fairly for their level of qualification. And so the answer is, there’s no single silver bullet, and I think we need for-profit entities.
You need not-for-profit entities funding research, like MAPS. I think you need not-for-profit entities funding access for marginalized communities. We certainly see a lot of that in the U.S. with military veterans and access.
Read more: 67% of PTSD sufferers drop diagnosis in first MDMA Phase 3 trial

The reception area at Field Trip’s clinic in Vancouver
And I think you need insurance — you need governments on board. You need insurers on board. I think through a collective effort — which we’ll get to, and I’ll explain why I think we’ll get there — you’re gonna be able to reach the most people possible. The reason I’m so confident is what we see in MAPS’s econometric studies of MDMA-assisted therapy, it should on average, save the U.S. healthcare system $100,000 per person.
We haven’t done the econometrics yet on ketamine-assisted therapy, but we know that for each improvement — the study suggests that for each one point improvement on a PHQ-9 score (a diagnostic tool for depression), productivity increases by 1.6 per cent. The studies suggest that people who have major depression or treatment-resistant depression tend to consume 30–40 per cent more medical resources than people who aren’t experiencing MDD or TRD. So the economics of providing access makes a lot of sense.
So on the insurance piece, given you have to be physician-referred in Canada, are there any insurers right now that cover your services?
There are extended health benefit plans that do cover the psychotherapy portion, so we bill in a way to try and maximize people’s ability to get reimbursed for the psychotherapy. For the ketamine, there’s really not much coverage
Do you anticipate any change on that? Especially because even if it’s an off-label use, it’s still being recommended by a doctor — it seems strange that there wouldn’t be coverage.
I think there will be change. But the reason that I hesitate is I think by the time that there’s enough evidence that people can support getting behind ketamine-assisted psychotherapy, you’re going to see the clinical trials for psilocybin — which are being specifically referred for treatment-resistant depression and major depression — come to fruition as well.
And because they will have a specific indication for psilocybin tied to mental health, I think you’ll see insurance coverage become much more accessible for those than ketamine.
Read more: Health Canada says patients should access medical psilocybin via clinical trials
Read more: US DEA suggests big increase of cannabis and psilocybin production for research
So there’s Field Trip Health, and then Field Trip Discovery. What kind of things is a Field Trip doing on the research side at the moment?
We’re looking to develop the next generation of psychedelic medicines. Psilocybin and MDMA are showing incredible promise, but one of the challenges with both of them, is that a session can be 4, 6, 8 or 10 hours. And because you need qualified people present during these sessions, it makes it very expensive.
So with one of our first compounds in a pipeline project, FT-104, we have something very similar to psilocybin, both objectively in terms of how it works in the brain, as well as objectively in terms of what the actual experience is like. But the duration of experience is about half that of psilocybin. You’re basically cutting the cost effectiveness in half.
And then we’ve also launched a new pipeline program, which is focused on psychedelics that have higher safety profiles. Overall, psychedelics are quite safe. But if they are used too frequently, they can create something called the 2B liability.
Psilocybin, LSD and tryptamines are kind of promiscuous, and they agonize a whole bunch of receptors. The 5HT2A receptor is the one that causes a psychedelic experience — you want to agonize that one. But 5HT2B receptor antagonized too much can create something called cardiac valvulopathy, basically a hardening of the cardiac valves. And so with our 200 series, we’re looking at ways to maintain the efficacy of the classic psychedelics, but reduce the potential 2B liability, which becomes particularly relevant to the as micro-dosing or chronic usage — as opposed infrequent, episodic uses — become more prevalent.
nick@mugglehead.com