Medline Canada is helping healthcare facilities such as hospitals and medical schools incorporate gamification elements into their training modules to improve outcomes and enhance clinician education.
These game-like components add fun and competition to the training, creating a more engaging and effective learning experience.
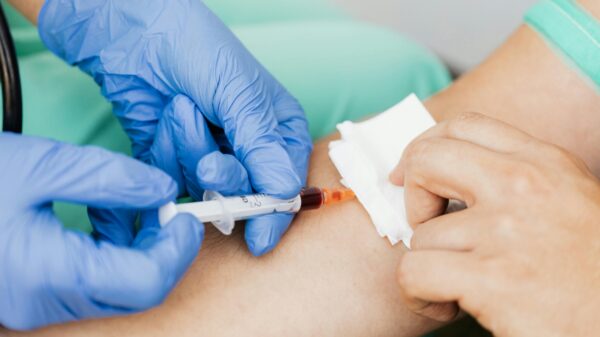
Senior director of clinical and training services at medical product manufacturer Medline Canada, Ruby Hartsell, provided an example where students were taught to wrap a surgical item, and then transformed it into a game wherein students competed against one another to see who could do it the fastest.
“At first, there’s a bit of a trepidation and a bit of giggling,” said Hartsell.
“What’s neat is that they surprise themselves, how well they know their work. It’s that brain-hand connection. They do a great job — it’s impressive to watch.”
The competition builds confidence and others observing the competition benefit from critiquing their peers, according to Hartsell.
Research performed at Carnegie Mellon University indicates there may be benefits to gamification.
Gamification of education can simplify goal setting for students by providing a clear framework for success, as games typically have well-defined rules and a straightforward path to earning points or advancing.
With technology becoming increasingly integrated in education, some schools are at the forefront of this trend, offering students opportunities to learn video game design and film production from a young age. These innovative approaches to learning are now being introduced in elementary schools.
Read more: FDA to reject medical device applications without cyberattack protection plans
Read more: Arthrex partners with Couchbase to help surgeons maximize patient outcomes
Partnership helps students learn through gamification
A partnership between the University of British Columbia’s faculty of medicine and Vancouver’s Centre for Digital Media has introduced the idea of games and apps that help medical students train. One of these games includes instructors controlling virtual patients as medical students use buttons to show how they would ask the patient questions.
Students noted the benefits of this technology, especially given the limitations on interaction posed by the pandemic. Also students from other countries indicated they could receive help in the virtual setting to learn and navigate the various cultural differences in Canada between patients and doctors, which is something they may not have been comfortable doing in person.
Cerebro is another example of a technology built to help students memorize brain structures for their neuroanatomy courses. Cerebro is a 3D game you play on a mobile phone. The player controls a robot named NeuRob, who acts as a guide through different regions of the brain and spinal cord. Players of the game can earn points by memorizing the structures, potentially aiding in their success on exams

Cerebro demo. Image via the Centre for Digital Media.
Read more: Dialogue Health Technologies new Wellness app promotes healthy habits, including sleep
Read more: Swarmio Media Holdings pushes Echo system to gamers on four continents
Gamification helps surgical patients recover
There is also gamification for surgeons and surgical patients. For example, research by the National Institutes of Health showed that gamification could also be used to incorporate machine learning technology to help patients optimize pre-operative risk, reduce in-hospital complications and hasten recovery.

Image from the National Institutes of Health.
During the controlled preoperative consultation for elective surgery, the patient’s baseline variables such as laboratory values, imaging, and medical and surgical history are recorded. Similarly, in gaming, an avatar serves as a representation of the player, and in this theoretical scenario, the avatar would be assigned initial fixed variables to predict surgical outcomes and guide the patient through pre- and post-operative challenges.
Each patient’s avatar would be completely individualized, displaying values to post-operative risks, such as wound complications, pulmonary issues or cardiac events. The patient will then be able to see and assess their own risks. This can be shown to a patient in clinic to start the conversation of operative risk, and help with decision making.
Follow Joseph Morton on Twitter
joseph@mugglehead.com