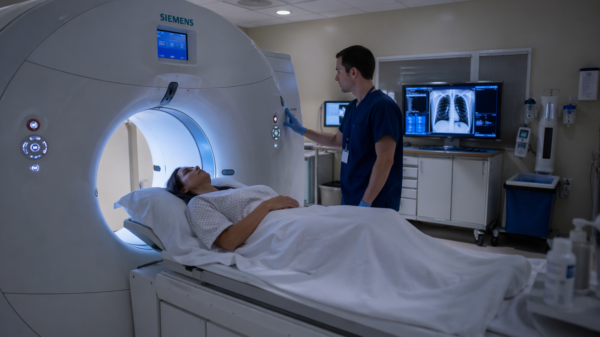
Canadian researchers have identified a way to accelerate the production of cancer fighting cell therapies, potentially lowering costs and shortening wait times for patients.
Scientists at the University of British Columbia and B.C. Children’s Hospital Research Institute say they have learned how to guide stem cells into becoming helper T-cells in the lab. Additionally, the advance could help bioengineers mass produce key immune cells for treatments.
Cell therapies have gained ground in recent years as doctors turn patients’ immune systems into “living drugs.” In the most common approach, clinicians extract a patient’s immune cells, modify them to target cancer, and then infuse them back. However, the process can take about two weeks and may fail if patients lack enough healthy cells.
That challenge has pushed researchers to pursue off-the-shelf immune therapies manufactured in advance. Consequently, scientists have focused on stem cells, which can multiply rapidly and transform into different cell types.
Ross Jones, a biomedical engineering research associate at the University of British Columbia, said stem cells offer a nearly limitless starting material. He explained that researchers can expand them in large numbers before directing them to become specialized immune cells.
Jones and his colleagues concentrated on helper T-cells, which coordinate immune responses. These cells detect threats and direct other immune cells to attack. Additionally, helper T-cells can make cancer cell therapies more effective by sustaining the immune response.
In the human body, stem cells naturally become helper T-cells through tightly controlled signals. However, recreating that process in a lab dish has proven difficult. Kevin Salim, a Ph.D. student at B.C. Children’s Hospital Research Institute, said producing this specific T-cell type outside the body remains technically challenging.
Read more: Breath Diagnostics completes install of advanced mass spectrometry system
Read more: Breath Diagnostics leaders promote their mission at Miami investment conference
New therapies could counter several treatment model bottlenecks
The team discovered that timing is critical. Specifically, they found that researchers must remove so-called “Notch signals” at certain stages to steer stem cells toward becoming helper T-cells. Consequently, the lab-grown cells behave much like those produced naturally in the body.
Salim said the newly generated helper T-cells act and function like their natural counterparts. Furthermore, early experiments suggest they can coordinate immune responses in ways that could strengthen cancer therapies.
The findings, published in a January study, open possibilities beyond oncology. Additionally, researchers believe the method could support treatments for autoimmune disorders, chronic inflammation, and transplant medicine.
Manufacturing cell therapies in advance could address several bottlenecks in current treatment models. Meanwhile, doctors would no longer depend solely on each patient’s immune cells. This shift could reduce production delays and improve consistency between batches.
However, researchers still need to test how these lab-grown helper T-cells perform once infused into patients. They must also determine which diseases respond best to this approach. Consequently, the team plans further preclinical studies before launching human trials.
The University of British Columbia is pursuing a patent for the technology. Additionally, the university is building a manufacturing facility designed to produce helper T-cells for clinical trials.
Clinical trials of stem cell-based immune therapies already operate in the United States. However, Canada has not yet launched similar trials using lab-manufactured stem cell immune products. Jones said the team hopes to begin Canadian trials using their helper T-cells in the future.