Artificial intelligence (AI) and machine learning (ML) can be used to detect and diagnose Polycystic Ovary Syndrome (PCOS), according to a new study released Monday by the National Institutes of Health (NIH).
Collaborating with a skilled NIH librarian, they identified potentially relevant studies. Out of the 135 studies screened, 31 were included in this paper. All of these studies were observational in nature and evaluated the application of AI/ML technologies in diagnosing patients.
Approximately half of the studies incorporated ultrasound images. The average age of the study participants across these investigations was 29 years old.
Among the subset of 10 studies that employed standardized diagnostic criteria to identify PCOS, the accuracy of detection ranged from 80 per cent to 90 per cent.
Researchers reviewed published scientific studies involving AI/ML to analyze data to diagnose and classify POCS, and discovered that the AI and ML based programs were capable of detecting the disorder.
“Across a range of diagnostic and classification modalities, there was an extremely high performance of AI/ML in detecting PCOS, which is the most important takeaway of our study,” said Skand Shekhar, M.D., senior author of the study and assistant research physician and endocrinologist at the NIEHS.
The authors emphasize that AI/ML-driven programs hold substantial promise in improving our ability to detect PCOS in women at an early stage, potentially leading to cost savings and alleviating the burden of PCOS on both patients and the healthcare system.
Read more: Biden secures 8 additional safety pledges from influential AI developers
Read more: AstraZeneca invests US$42M in Verge Genomics AI drug discovery platform
Researchers look back at peer-reviewed studies over the past 25 years
The authors of the study have proposed a comprehensive approach, combining large-scale population studies with electronic health data analysis, to pinpoint sensitive diagnostic biomarkers that could enhance the detection of PCOS.
Janet Hall, M.D., senior investigator and endocrinologist at the National Institute of Environmental Health Sciences (NIEHS), a subdivision of the NIH, said in a statement that the effectiveness of AI and machine learning in PCOS detection was even more impressive than she had originally thought.
“Given the large burden of under- and mis-diagnosed PCOS in the community and its potentially serious outcomes, we wanted to identify the utility of AI/ML in the identification of patients that may be at risk for PCOS,” said Hall.
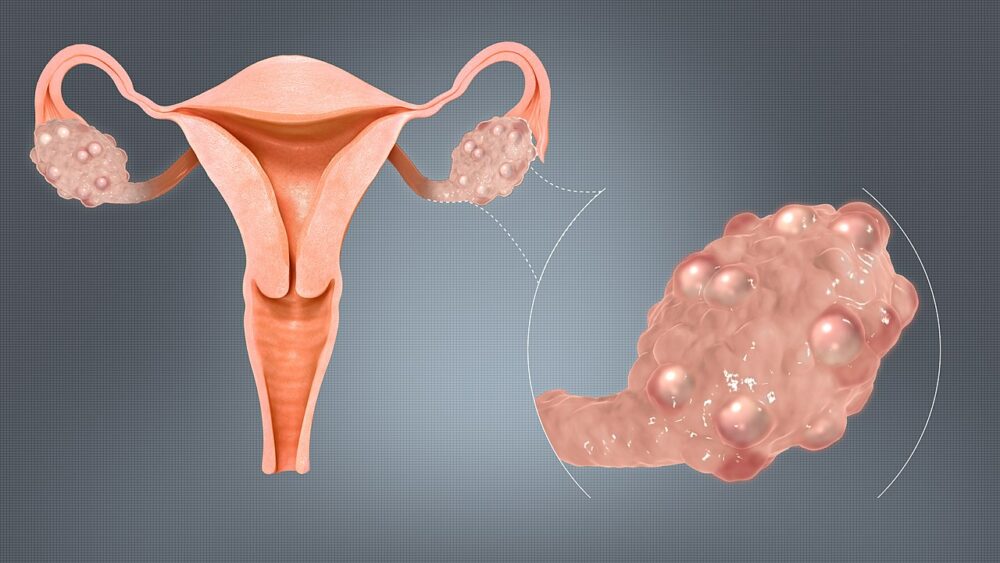
Diagnosis of PCOS relies on established standardized criteria that have evolved over time. Typically, it involves the evaluation of clinical indicators like acne, excessive hair growth and irregular menstrual cycles, alongside laboratory assessments such as elevated blood testosterone levels, and radiological findings like the presence of numerous small cysts and increased ovarian volume observed through ovarian ultrasound.
However, PCOS symptoms can sometimes overlap with other conditions like obesity, diabetes and cardiometabolic disorders, leading to frequent instances of misdiagnosis or underdiagnosis.
“PCOS can be challenging to diagnose given its overlap with other conditions,” said Shekhar.
“These data reflect the untapped potential of incorporating AI/ML in electronic health records and other clinical settings to improve the diagnosis and care of women with PCOS.”
PCOS arises due to ovaries functioning abnormally, frequently resulting in elevated testosterone levels. This condition can manifest as irregular menstrual cycles, acne, excess facial hair, or hair thinning on the scalp. PCOS is also the most common hormone disorder among women between the ages of 15 and 45, according to the NIH.
Additionally, women with PCOS face a higher likelihood of developing various health issues, including type 2 diabetes, sleep disturbances, psychological challenges, cardiovascular complications and other reproductive disorders such as uterine cancer and infertility.
joseph@mugglehead.com